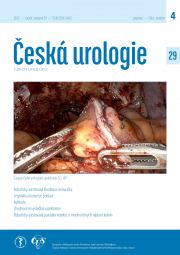
Robot-assisted resection of renal tumour – our current most common technique – video.
Milan Hora, Ivan Trávníček, Petr Stránský, Adriena Bartoš Veselá, Tomáš Pitra, Hana Sedláčková, Petr Stránský Jr, Dominika Šiková, Kseniia Khomenko, Blanka Drápelová, Jitka Voráčková, Jiří Ferda, Kristýna Pivovarčíková.
Aim: To present on video our current most used technique of robot-assisted resection of renal tumour (RR).
Material: We performed 274 RRs between June 2020 and November 2024. Our technique is based on a modification of conventional laparoscopic renal resection, of which we performed 599 between August 2004 and May 2020. RRs currently account for over one third of the surgical procedures for kidney cancer at our institution. Laparoscopic (rarely robotic assisted) nephrectomy is almost as frequent. Open resection accounts for about 17% and open nephrectomy for slightly less. Open resections are mainly indicated for more complex tumours, for tumors with significant \"toxic\" fat capsule, and when combined with other procedures, mostly for intestinal malignancies. RR is routinely performed by two console surgeons, occasionally by two additional ones.
Operation technique: General anaesthesia. Optional urinary catheter inserted. Lateral position 60-70°. Upper limbs extended in front, close together. Operative field prepared for eventual lumbotomy. Transperitoneal approach. The capnoperitoneum is created with a Veres needle, CO2 pressure 12 mmHg. Assist port 12 mm slightly lateral to the umbilicus. Four 8-mm robotic ports are inserted pararectally under visual control. Four-arm daVinci Xi robotic system is inserted. Ports craniocaudally: 1. ProGrasp, 2. bipolar grasper (bipolar forceps Maryland or more often fenestrated) or monopolar curved scissors (Hot shears) according to the operated side and the dominant hand of the operator, 3. camera 30°, 4. the second of the mentioned instruments from port 2. The scissors are alternated with a needle driver, usually the Large SutureCut needle driver. In the Toldt line, the peritoneum is opened, the colon is retracted medially, and the Gerota fascia is opened medially from the kidney. The necessary part of the kidney is dissected from the fat capsule for good access to the tumour. The tumour is verified sonographically with a drop-in probe inserted through the assistant port. Scissors can be used to mark the line of resection on the kidney. The ureter is verified and the hilar vessels are released. The artery(s) or necessary branch is bypassed with tubing and clamped with the SCANLAN® robotic endo-bulldog. Only in central tumours is the vein also clamped. Knowledge of the topographic anatomy of the vessels from two-phase CT angiography is very helpful at this stage. The effectiveness of ischemia is verified by Doppler; exceptionally (especially in selective clamping of the artery branches) by NIR imaging with FireFly® with administration of indocyanine green - Verdye® 1.25-2.5 mg. The tumour is resected with cold scissors with a rim of healthy tissue. Suturing of the base is performed with an absorbable self-anchoring barbed suture (V-Loc® 90, size 3-0, 1/2 needle 26 mm). The edges of the kidney are mattress sutured with another suture, tightened with Absolok® AP300 absorbable clips (polydioxanone PDS, size ML) – \"sliding clips\" technique. The second layer of the parenchyma is sewn with simple continuation stitches, mostly without continuous anchoring. For more superficial tumours, a straight suture of the parenchyma is performed, including anchoring of the base. The hilar vessels are released. Eventual residual bleeding is usually treated with a larger needle - V-Loc® 90 2-0 needle 37 mm. Exceptionally, woven cellulose Surgicel® is applied to the suture. We have eliminated tissue adhesives from the armamentarium. The Gerota fascia defect is closed with V-Loc® 90 3-0 suture. The tumour is placed in an Endocatch® Gold extraction bag. A drain is usually not used. If used, then Penrose inserted after the robotic port 1 or 2 (taken craniocaudally). The tumour is extracted through the dilated port in the lower abdomen after the robotic port 3 and closed with Vicryl® suture introduced with a Berci fascial port closure forceps. Smaller tumours are extracted at the assist port site without the need for closure. The patient is mobilized early, only if it is necessary to release the whole kidney is he left on bed rest for 2-3 days. The slide is stained with black ink at the base.
Video: Lasting 6 min 17 sec, it shows the above technique for left-sided resection, the surgeon has left hand dominance. Procedure combined with fenestration of parapelvic cysts. Clamping of the main artery used, single layer suture of the resected kidney with treatment of residual bleeding.
Conclusion: It has completely replaced the laparoscopic approach. The key points are predominant transperitoneal approach, knowledge of vascular anatomy from CT angiography, extent of renal release according to tumour localization, clamping of the artery with endo-bulldog, verification of ischemia efficiency with Doppler, cold scissors, absorbable self-anchoring sutures and absorbable PDS clips, suture of Gerota\'s fascia, no use of drainage, staining of the base of the specimen.
Key words: kidney tumour, resection, laparoscopy, robot

Variant of urethrovesical anastomosis during robot assisted radical prostatectomy – video.
Schraml J, Hlavička M, Hora M.
Ces Urol 2024; 28(1): 10-12
Introduction: There are many methods of performing a urethrovesical anastomosis during robot assisted radical prostatectomy, while there are no data from prospective randomized studies to prefer one specific technique. The aim of this video is to present the technique used at the workplace of the main author of this work.
Methodology description: A trans- or extraperitoneal antegrade radical prostatectomy is performed in the Trendelenburg position with the DaVinci Xi robotic system – the prostate is separated from the bladder neck and dorsally from the neurovascular bundles. The operation in the video is performed by a right-handed surgeon. The video begins by cutting the Santorini plexus and the urethra in its 5/6 circumference with scissors, the urethra is left dorsally to prevent its retraction caudally into the pelvic floor. The bleeding Santorini plexus is sutured with a Stratafix® Monocryl 3-0 continuation self-anchoring suture, and the thread is left in the abdominal cavity fixed with a needle to the anterior abdominal wall for further use. A second identical suture is placed on the non-retracted urethra at no. 5. Using a cutting needle (Larger SutureCut needle driver) the urethra is interrupted. This is followed by a urethrovesical anastomosis without supporting reconstruction of the levator ani muscle. Three thread turns are made without tension on No. 5-8 and only then the stitch is gradually tightened. The anastomosis at No. 8-12 is completed, and the stump of the Santorini plexus is sutured ventral to the urethra. The anastomosis is closed with the remainder of the first suture from No. 5 in the ventral direction to No. 12. The needles of both sutures are cut and both ends of the self-anchoring sutures are still tied.
Comment on the technique: The methodology has been used for over 10 years in more than 2,000 cases with satisfactory functional results, but the results have not been analysed in a high quality study. We do not routinely perform posterior reconstruction, this is also a given historically, when we did not perform it even in open procedures and we did not have more frequent complications of urinary continence. We perform posterior supportive reconstruction only very exceptionally when there is a large spacer defect after removal of the prostate, and in this case our intention is to reduce the tension of the subsequent anastomosis. We perform the actual interruption of the urethra at the apex of the prostate with an effort to preserve the puboprostatic ligaments as much as possible, especially their distal fibres, which also go into the external bundle. By subsequently taking this area into a suture, we carry out a certain reconstruction of the suspension apparatus in the neck of the bladder and there is no decrease in this area. We consider this front-upper reconstruction to be more physiological than performing a routine posterior support reconstruction. Our functional results, including economic aspects, have not forced us to change our strategy for more than 10 years.
Conclusion: The video presents one of the possible variants of urethrovesical anastomosis during robotic-assisted radical prostatectomy.

Roborically assisted retroperitoneoscopic renal tumor resection - case report
Václav Krejčí, Kamil Belej, František Chmelík, Jiří Heráček, Miroslav Záleský
Ces Urol 2022, 26(3):162-164
Introduction: The retroperitoneoscopic approach is advantageous from the point of view of its minimal invasiveness, on the other hand, its disadvantage is the limited space, which can make the actual surgical preparation and treatment of the resection area technically more difficult.
Material and methods: In the video presentation, we show the case of a 57-year-old man with abdominal obesity (120 kg, BMI 40), who was diagnosed with a 6 cm tumor on the dorsal side of the convexity of the upper pole of the right kidney based on ultrasonography and subsequent CT examination (RENAL score 9p). The tumor was successfully removed by robotically assisted retroperitoneal resection with minimal blood loss and without intraoperative and postoperative complications.
Conclusion: The retroperitoneoscopic approach is advantageous in the case of a kidney-sparing procedure in the presence of dorsally placed kidney tumors, especially in obese patients and patients after previous operations in the peritoneal cavity.

Laparoscopic transposition of crossing vessels ("vascular hitch ") in ureteropelvic junction obstruction - a case report
Radim Kočvara, Josef Sedláček, Marcel Drlík
Ces Urol 2021, 25(4):231-235
Aim of the study: Crossing vessels of the lower renal pole are found in 10-15 % of children with ureteropelvic junction (UPJ) obstruction, and in more than half of older children and adolescents (2). The obstruction, caused by external pressure of the vessels on the UPJ or proximal ureter, is often intermittent and manifests by recurrent and even colic pain. In an acute condition, we can detect a high grade hydronephrosis that may disappear after resolution of the acute episode. The aim of this video is to show intraoperative evaluation and policy in hydronephrosis accompanied by crossing vessels and performance of laparoscopic repair without opening of the urinary tract according to Hellström (1).
Methods: Doppler ultrasound examination is of paramount importance in detection of crossing vessels of the lower renal pole. On intravenous urography, a globular shape of the pelvis with a flat bottom and calyceal dilatation has been described in crossing vessels (3). Surgery is considered in confirmed UPJ obstruction based on symptoms and findings on dynamic renal scintigraphy or on intravenous urography with furosemide. Functional magnetic resonance urography is a good alternative, moreover, detecting the crossing vessels (4) CT urography is inappropriate in children because of a high radiation burden. If the vascular hitch is being considered, it should be born in mind, that an "extrinsic obstruction ", caused by external pressure of vessels or adhesions, may be accompanied by an "intrisic" obstruction, a real UPJ or proximal ureter stenosis with pathohistological changes in the ureteric wall. In this case a dismembered repair should be performed (3). Hellström described elevation and adventitial fixation of the vessels to the renal pelvis outside the region of UPJ in 1949 (1). Chapman proposed to stabilise the vessels in the new position by wrapping them in the pelvic wall. This method has gained popularity in selected patients especially after introduction of laparoscopy as an easier alternative to technically demanding laparoscopic suturing in dismembered pyeloplasty (5-7). The Chapman modification has been used in our case as well. Surgery has three phases. First, releasing of crossing vessels from the pelvis and ureter is performed and the vessels are freely pulled cranially outside the UPJ region. The second phase should prove free passage of urine after liquid infusion and furosemide administration. It is necessary to wait 10 minutes to achieve full diuretic effect. If UPJ obstruction persists at visual control, then a dismembered repair is to be used (8). During the third phase, the vessels are wrapped within the anterior pelvic wall at the elevated position according to Chapman.
Results and discussion: An 8-year-old boy was investigated because of intermittent abdominal pain. Grade II hydronephrosis of the right kidney with crossing vessels to the lower pole was detected on ultrasound and Doppler imaging. Diuretic scintigraphy with 99mTc-MAG3 has shown symmetrical differential renal function (48 %) and delayed drainage of the radionuclide pointing to a partial obstruction of the right kidney. The right kidney was laparoscopically exposed in conventional transperitoneal way with three 5mm trocars inserted at umbilicus, above umbilicus in the midline and pararectal to umbilicus. The crossing vessels were released from the enlarged pelvis, UPJ and proximal ureter to enable free movement up and down behind the vessels ("shoeshine manoeuvre "). After i.v. liquid infusion, the vessels were elevated from the UPJ region and 10 mg furosemide i.v. was administered. A good passage of urine from the pelvis to the ureter across the UPJ was confirmed. The vessels were wrapped into the pelvic wall well above the UPJ using two absorbable polyglactin 4/0 sutures. Length of surgery 115 min. Stenting was not necessary, therefore, no worry of stent syndrome and of necessity for additional anaesthesia to remove it. Postoperative course was uneventful, pain settled and dilatation of the pelvicalyceal system decreased at 3- and 12- months follow-up. Doppler imaging showed adequate cranial deflection of the crossing vessels and good perfusion of the kidney. The laparoscopic vascular hitch was first published by Meng and Stoller in 2003 (6). Several articles have been published proving safety of the procedure. Its success rate (97,5 % ± 1,6 %) is comparable with dismembered pyeloplasty (9). The pros are: unstented repair, shorter length of surgery and hospital stay (9, 10).
Conclusions: Laparoscopic transposition of crossing vessels is a good alternative of dismembered pyeloplasty in selected patients with intermittent hydronephrosis once concomitant "intrinsic" cause of UPJ obstruction has been excluded. It is a stent free procedure with a shorter operative time and shorter hospitalization.

Our technigue of robot-assisted radical cystectomy in women
Miroslav Štursa
Ces Urol 2021, 25(3):173-174
Štursa M. Our technique of robot-assisted radical cystectomy in women.

Inferior vena cava lesion as a complication of laparoscopic radical nephroureterectomy with retroperitoneal lymphadenectomy
Lenka Plincelnerová, Milan Čermák, Lukáš Fišer, Ágnes Juhász, Jiří Kočárek
Ces Urol 2021, 25(2):90-93
Introduction: Upper urinary tract tumors occur in 5-10 % of all urothelial tumours. The prognosis is poor due to late clinical manifestation resulting in late diagnosis. Radical laparoscopic nephroureterectomy is considered gold standard treatment. In case of high risk tumors, retroperitoneal (paraaortic, paracaval) lymphadenectomy is carried out. Inferior vena cava lesions come as a rare, but serious complication of this type of surgery. Clinical case: We present a case of a 55 years old female patient with oncological duplicity: tumour of the renal pelvis, topic of this presentation, and an oesophageal tumour (epidermoid carcinoma classified as pT2pN0Mx, R1). In 2018, the patient underwent total oesophagectomy, D2 lymphadenectomy and a posterior mediastinal lymphadenectomy with gastrooesophagoanastomosis. On restaging CT scan 2 years after the surgery, there was a newly discovered unclear finding on the right kidney, which was suspicious of a metastatic invasion. In differential diagnosis, either abscess or a primary kidney tumor were considered. Due to the inconclusive imagery, we performed another early CT check-up, progression on the right kidney and on the retroperitoneal lymph nodes was described. Diagnostic ureterorenoscopy including cold biopsy and wash-out cytology was performed. Eventhough the histopathological and cytological examination wasn´t helpful, the endoscopy showed the expansion to be of suspicious appearance and therefore right sided radical nephroureterectomy with retroperitoneal lymphadenectomy were recommended. Laparoscopical approach was chosen for surgeon´s skills. The surgery was complicated by an injury of the inferior vena cava. The situation was fortunatelly recognized perioperatively and therefore the primary suture could be performed. We proceeded according to the rule of "3 P" - Pressure, Panic, Port - Compress the laesion immediately to stop the bleeding and increase the intraabdominal pressure, keep calm and insert another port for additional instruments to fix the lesion. On our recording, all these steps are visible: compression of the lesion, suction of the bleeding and suture, which is performed with a Prolene 3/0 suture. Surgery took 4 hours and 15 minutes and there was less than one litre of blood loss. Postoperative hemoglobin level was sufficient and there was no need for transfusion. The complications are classified as Clavien-Dindo 1. Intramural part of the ureter was removed by Collins knife. The subse quent postoperative period was uncomplicated. The drainage was removed on the the third day and the patient was discharged on the eighth day. On the histopathological examination, there was a sqamous carcinoma of the renal pelvis described, with positive lymph nodes (pT3pN2, grade 3). Primary sqamous carcinoma of the renal pelvis is a rare histopathological finding. It appears in only 1 % of all urothelial malignancies, but it is the most frequent histopathological variation of urothelial tumours. The patient was passed to the complex oncological center, where she was already treated for the earlier diagnosed oesophageal tumour. She received adjuvant chemotherapy (Cisplatinum + Gemzar, 5 cycles in total). The adjuvant chemotherapy was eventually interrupted due to hematotoxicity. The follow-up CT scan revealed generalisation to lungs, right suprarenal gland and paraaortic lymph nodes.
Conclusion: Retroperineal lymphadenectomy represents an important step in surgical treatment of different urological tumours however vena cava laesions can come as a complication of surgery. There can be other iatrogenic causes, for example ureteral stent insertion. Inferior vena cava lesions can be fatal and the best way to handle this complication is to recognize the laesions perioperativelly and to perform primary suture.

Fast and effective percutaneous lithotripsy using "Bernoulli effect"
Tomáš Hradec, Vladimír Vobořil, Ondrej Kaplán, Lucie Vávřová, Libor Zámečník, Tomáš Hanuš
Ces Urol 2021, 25(1):15-16
The choice of treatment method for medium size urolithiasis (10-20 mm) is not always easy. Extracorporal shockwave lithotripsy might create multiple large residual fragments, which might cause obstruction of the upper urinary tract. Flexible ureterorenoscopy might be a long, complicated procedure with the risk of infectious complications. Percutaneous lithotripsy (PCNL) is very effective, but the use of standard size PCNL instruments (24-30 CH) might be too invasive and require prolonged hospitalisation. Mini-PCNL (16 CH) with the use of "Bernoulli" or "vacuum cleaner" effect for irrigation of fragments from the upper tract seems to be an excellent choice of treatment. It is fast, effective and it does not require use of any expensive extraction devices. We would like to present our experience with mini-PCNL using Karl Storz MIP instruments. The advantage of this method is small diameter access, minimal blood loss and single step dilatation, without traumatisation of the upper urinary tract. The fragmentation is easily performed by standard Ho:YAG laser. We have used this technique in seven patients with the average stone size of 12 mm. Total procedure time, including insertion of ureterical catheter and rotation of the patient into the prone position was 68 minutes on average. We identified residual fragments smaller then 2 mm on a CT scan early after procedure in one patient. All the other patients were stone free right after the surgery. The procedure did not lead to significant blood loss, which would require blood transfusion in any of the patients. Mini-PCNL with a 16 CH access tract and the use of "Bernoulli effect" for fragment evacuation, is a safe and very effective treatment method for medium size stones.

Laparoscopic nephron-sparing surgery in a patient with multiple tumours in a solitary kidney
Michael Pešl, Květoslav Novák, Petr Macek, Jan Novák, Pavel Dundr, Tomáš Hanuš
Ces Urol 2021, 25(1):13-14
Aim: To present a video of laparoscopic kidney resection in a patient with multiple tumours of a right sided solitary kidney.
Material and methods: Female patient, 63 years of age, after open transperitoneal nephrectomy on the left, histology confirmed clear cell renal carcinoma (pT2b G3). Two new tumours in the right solitary kidney were found during staging CT. The patient was indicated for laparoscopic nephron-sparing surgery. We found another five small tumours during the procedure. PADUA score: 2x, 9a, 5x, 7a. We resected all the tumours into macroscopicaly negative margins from four resection defects. We used selective clamping (WIT 19 min) during resection of the biggest tumour. We used V-Loc™ stitch to close the defects.
Results: Blood loss was up to 100 ml, no significant renal function impairment was detected. No postoperative complicaions were present. Total hospital stay was 10 days. Result of histopathologic assesment was clear cell carcinoma pT1a G2, there was positive surgical margin in one tumor (the biggest tumour, 12x11 mm) of 2 mm in size.
Conclusions: Laparoscopic nephron-sparing surgery of solitary kidney is a safe, feasible, but technically demanding method of multiple kidney tumours treatment. The patient is free of disease after 12 months from the surgery.

Matějková M. Robotic-assisted vesicovaginal fistula repair: step by step.
Ces Urol 2020, 24(1):15-17
Introduction: Vesicovaginal fistula is a pathological communication between the bladder and the vagina. It most commonly occurs as a postpartum complication in developing countries and as an iatrogenic postoperative complication in developed countries. The presented video illustrates the surgical procedure in individual steps.

Drlík M, Kočvara R. Laparoscopic transperitoneal reconstruction of retrocaval ureter – a case report.
Ces Urol 2019, 23(4):292-294
The authors present a case report of a 12-year‑old girl with a symptomatic retrocaval ureter. A standard ureteral anteposition in front of vena cava with the excision of retrocaval ureteral segment was performed using a transperitoneal laparoscopic approach. It is the first case of laparoscopic reconstruction of retrocaval ureter in Czech literature.

Hora M, Trávníček I, Stránský P, Nykodýmová Š, Mlynarčík M, Ferda J, Kacerovská D, Hes O. VEILND (VideoEndoscopic Inguinal Lymph Node Dissection) in penile cancer ≥pT1G2 and cN0.
Ces Urol 2019, 23(3):183-185
Introduction: Invasive diagnosis is indicated in penile carcinoma ≥pT1G2 cN0 (palpable or controversially palpable non-tumorous inguinal nodes). Either a scintigraphically labelled sentinel node (DSLNB) biopsy with false negative risk over 10% or more accurate but more invasive modified inguinal lymphadenectomy (ILND), done usually as open surgery. In particular, modified ILND is indicated in associated risk factors (more aggressive histology, positive inguinal nodes in FDG PET MRI / CT, in younger men). To reduce complications, we introduced a mini-invasive "laparoscopic" ILND in 2017. We present our experience with methodology VEILND.

Schraml J, Hlavička M, Broul M, Cihlář F. Minimally invasive closure of a vesicovaginal fistula using robotic single‑site surgery
Ces Urol 2019, 23(2):97-100
We report our experience with the closure of a vesicovaginal fistula using a highly minimally invasive technique - using a single‑port approach with the da Vinci Xi robotic system: a video.

Kočárek J, Hoření E, Chmelík F, Matějková M, Čermák M, Heráček J. The robotic intracorporal Hautmann orthotopic neobladder.
Ces Urol 2019, 23(2):95-96
Introduction: The daVinci robotic system with modern EndoWrist tools enables a miniinvasive approach to intracorporeal reconstruction of orthotopic neobladder after cystectomy. Description of the clinical case: We performed 42 robotic radical cystectomies since January 2010 to June 2018. We had used the robotic system daVinci standard until December 2013, then we used daVinci Si. During procedures patients were positioned in 30 degrees Trendelenburg position. After the ablation phase of cystectomy orthotopic neobladder was created intracorporally, in 5 cases according to Hautmann. We are presenting the Hautmann neobladder reconstruction in which we have used about 60 centimeters of preterminal ileum. Bowel continuity was restored by continuous end to end suture. Excluded bowel loop was remodeled after partial detubulization to W shape, then we sutured it to the remainder of urethra. The non-tubularized afferent parts of bowel loop were attached to stented urinary ducts. Mean age of the patients was 62 years (56-68), mean BMI was 24 (17-32). Mean time of surgery procedure was 150 minutes (120-200) and mean time of hospital stay was 10 days (8-14). Three weeks after, the surgery cystogram with cathether removal was performed. In postsurgery period, we did not register prolonged bowel passage, neobladder leak or any serious complications.

Balík M, Hušek P, Špaček J. Robotic‑assisted radical cystectomy in a woman.
Ces Urol 2019, 23(1):16-18
A short video is presented of robotic‑assisted radical cystectomy, hysterectomy, adnexectomy, and prophylactic appendectomy with intracorporeal Bricker diversion.

Hora M, Stránský P, Pitra T, Ürge T, Trávníček I. Laparoscopic radical cystectomy with open ureteroileostomy
Ces Urol 2019, 23(1):13-15
The aim of this work is to present our approach to laparoscopic radical cystectomy (LRC), which we introduced in ERAS implementation. ERAS (Enhanced Recovery After Surgery) in Radical Cystectomy (RC) includes 22 measures, one of which is the use of mini‑invasive approaches. For these reasons, we have implemented laparoscopy for RC, although not all ERAS measures have been introduced. Pure laparoscopy versus robotic has limited possibilities for intracorporal diversion, so we combine laparoscopic ablation phase with extracorporal diversion. Only in RC with concomitant unilateral nephrourectomy (mostly for non‑functioning kidney in advanced megaureter) and ureterocutaneostomy is performed completely laparoscopically. RC with orthotopic neobladder, we are still perform entirdy openly.